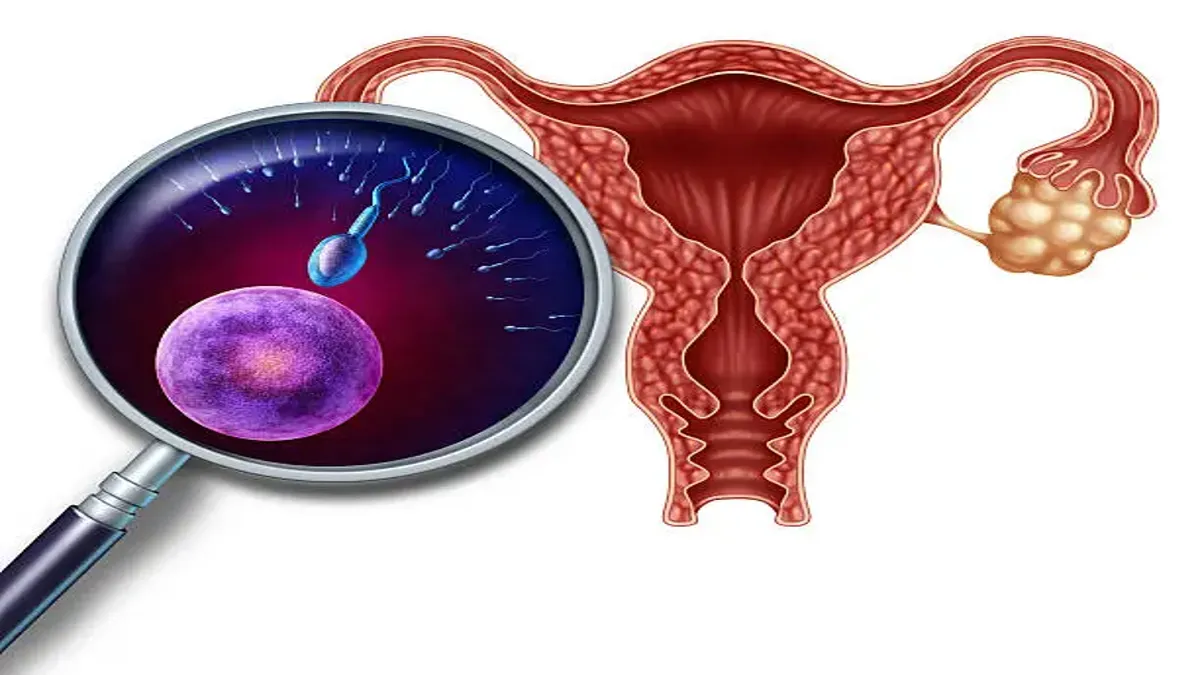
A blighted ovum, also known as an anembryonic pregnancy, is one of the most common contributors to early miscarriage, but few expect it when those first hopeful signs of pregnancy begin. In the first 100 words: the condition occurs when a fertilized egg implants in the uterus and the gestational sac begins to grow—with rising hormones and typical early-pregnancy symptoms—yet no embryo ever forms within it. This empty sac is often not discovered until an early ultrasound scan, typically between six and nine weeks. To a patient expecting to hear a heartbeat, the silent stillness of the screen can feel devastating. The positive home test, the nausea, the tender breasts—all seemed to suggest a normally developing pregnancy. Instead, the scan reveals an absence that can feel medically clinical but emotionally enormous.
The experience is far more common than most people realize, accounting for a significant portion of first-trimester miscarriages. Because symptoms mimic a healthy pregnancy, people often continue to believe everything is progressing as it should, unaware that chromosomal abnormalities halted development long before the doctor ever touched the ultrasound probe. For many, the diagnosis arrives not with warning signs but during routine care, creating a sudden collision between anticipation and loss.
This article takes readers through the science, the statistics, the options, and the lived experiences surrounding blighted ovum. Through carefully structured sections, an in-depth interview, and insights from medical experts, it examines not only the biology but also the complexity of navigating early pregnancy loss in a world that rarely speaks openly of it.
Understanding a Blighted Ovum
A blighted ovum is defined by the presence of a gestational sac without an embryo. The egg fertilizes normally and implants in the uterine lining. Hormone levels rise. The sac grows. Early placenta-like tissue may form. But the embryo itself either never develops or stops growing so early that no fetal pole is ever visible, even with sensitive transvaginal ultrasound. This disconnect between the hormone-driven signals of pregnancy and the absent embryo is what makes the diagnosis both medically straightforward and emotionally disorienting.
Clinicians often emphasize that a blighted ovum is not caused by behavior, diet, or lifestyle. Instead, most cases stem from chromosomal abnormalities in the fertilized egg—errors that occur at random, often in the very first divisions of embryonic life. The body, responding to these genetic problems, halts embryonic development even as the surrounding structures continue momentarily. This is why many patients still have positive tests and classic symptoms. The sac’s continued growth gives the impression of progress, masking the underlying reality until imaging reveals the truth.
How Common It Is: The Scale of Early Loss
Blighted ovum belongs to a large category of early pregnancy losses, many of which occur before a person even realizes they are pregnant. Within clinically recognized pregnancies, miscarriage affects an estimated one in five. A blighted ovum is believed to cause a large share of these early losses, sometimes cited as up to half of first-trimester miscarriages. Although percentages differ across clinical settings, the consistent message is clear: this form of miscarriage is far more widespread than its public awareness.
Statistical Overview of Blighted Ovum
| Category | Estimate |
|---|---|
| Share of known pregnancies ending in miscarriage | Around 10–20% |
| Portion of early miscarriages attributed to blighted ovum | Up to 50% |
| Prevalence in one first-trimester clinical sample | ~15% |
The frequency can be startling for anyone experiencing the diagnosis for the first time. Many pregnancies lost to this process occur so early that they resemble a slightly delayed or heavier menstrual cycle. Others progress far enough for the person to have formed early attachments, articulated hopes, and mapped out tentative plans—making the discovery of an empty sac profoundly distressing.
Causes and Contributing Factors
The predominant cause of a blighted ovum is chromosomal abnormality. When the genetic material from egg or sperm is flawed—extra chromosomes, missing chromosomes, or errors in early replicating cells—the embryo cannot progress. And yet, paradoxically, the gestational sac may grow for a brief period, driven by hormonal signals from the developing trophoblast tissue. This creates the illusion of a viable pregnancy.
Experts stress that this is a natural safeguard. The body recognizes the embryo cannot form normally and stops its development early, preventing more complex complications down the line. Importantly, because these abnormalities occur at random, they rarely indicate an underlying fertility problem. They also are not preventable: no vitamin, diet, or lifestyle change can eliminate the chance of chromosomal mispairing.
Three medical experts summarize the matter clearly:
“Most anembryonic pregnancies reflect random chromosomal errors, not parental health or behavior.”
“It’s a biological misfire, something that happens long before an ultrasound could detect life.”
“Patients always ask what they did wrong. The answer—truly—is nothing.”
Such guidance can be crucial in dispelling guilt and shame, emotional burdens that often accompany early pregnancy loss even when biology, not behavior, is responsible.
Recognizing a Blighted Ovum
Because the body continues to produce pregnancy hormones, symptoms frequently resemble a typical early pregnancy. People may feel nauseated, fatigued, tender-breasted. They may have strong positive urine or blood tests. The absence of an embryo does not immediately change these biochemical markers.
Only later—sometimes weeks later—do signs begin to shift. For some, pregnancy symptoms fade unexpectedly. For others, bleeding or cramping emerges. However, for many, the diagnosis becomes evident only during routine ultrasound. At the point when a fetal pole or heartbeat should appear, the gestational sac remains empty. A repeat scan sometimes confirms the finding, ensuring that dates are accurate and avoiding the risk of incorrectly diagnosing a very early pregnancy.
This moment—silent ultrasound, no embryo—is often described as surreal. Many patients report a sense of emotional whiplash: one moment anticipating the visible spark of new life, the next confronted with stillness.
Diagnosis and Confirmation
Diagnosis relies primarily on ultrasound imaging. When the sac reaches a size at which an embryo should be visible, its emptiness becomes diagnostic. Clinicians often wait for a follow-up scan if dates are uncertain, ensuring that what appears to be an empty sac is not simply too early for visualization.
Hormone levels, particularly hCG, may provide clues but cannot confirm the diagnosis alone. hCG may rise initially, plateau, or even remain elevated briefly despite absent embryonic development. Only imaging provides clear evidence.
The confirmation can be medically simple yet emotionally heavy. Some people request copies of the ultrasound images, even if the sac is empty. Others require time to absorb information, seeking space for questions that range from medical to existential.
Management Options
Once confirmed, individuals face three primary paths for completing the miscarriage.
Management Strategies
| Method | Description | Benefits | Considerations |
|---|---|---|---|
| Natural passage | Allowing the body to miscarry spontaneously | Avoids medical or surgical intervention | Timing unpredictable; may involve extended bleeding |
| Medical management | Medication triggers expulsion of gestational tissue | Faster, more controlled | Can involve intense cramping; requires monitoring |
| Surgical management (D&C) | Removal of tissue via minor procedure | Quick resolution; medically predictable | Procedural risks, though low in experienced hands |
The choice depends on personal values, medical history, emotional readiness, and physical symptoms. Some prefer the privacy and natural timing of spontaneous miscarriage. Others seek the clarity and completion that comes with medical or surgical intervention. Clinicians typically support whichever route aligns best with the patient’s physical safety and emotional well-being.
Interview Section
“The Ultrasound Room Was Too Quiet”
Date: Late January morning
Location: A metropolitan women’s health clinic
Atmosphere: Soft fluorescent lights, muted monitors, the scent of antiseptic and paper gowns
I meet Dr. L., a reproductive medicine specialist who has counseled countless patients through the complexities of early pregnancy loss. I sit across from her in a small consultation room tucked behind the imaging suite. The hum of equipment filters through the door. She rests her hands calmly on her lap as she begins to speak.
Scene-setting paragraph:
The hallway outside is busy with quiet footsteps, but here the air feels still. A sonographer walks past with a folded towel, another with a printout of a scan. These walls have held joy—positive scans, first heartbeats—but they have also held silence. Dr. L. has spent years guiding patients through the abrupt shift from anticipation to loss, particularly in cases of blighted ovum.
Q: When patients first hear the diagnosis, what do you notice most?
A: She exhales slowly. “The silence. People expect a heartbeat, a flicker of life. When the room is quiet, it hits them instantly. It’s not confusion—it’s recognition that something has gone very wrong.”
Q: How do you explain what caused it?
She leans forward. “I tell them the truth. It’s usually chromosomal. Random. A biological error, not a failure on their part. That knowledge helps release guilt, even if it doesn’t erase the pain.”
Q: What emotional responses are most common?
She pauses. “Shock, grief, frustration. Many feel betrayed by their own bodies, especially because their symptoms felt so real. I validate those feelings—they’re legitimate and important.”
Q: What guides the decision between natural and medical management?
She rotates a pen gently. “Safety first. But beyond that, it’s deeply personal. Some want the experience to unfold naturally. Others want closure quickly. My role is to present options clearly, without pressure.”
Q: What do patients most often fear afterward?
Her voice softens. “That it will happen again. And I reassure them: most go on to have healthy pregnancies. A blighted ovum is usually a one-time event.”
Post-interview reflection:
Walking out of the clinic, I am struck by the quiet compassion woven into Dr. L.’s work. In rooms where hope and heartbreak often share the same day, her steady presence becomes a small anchor—a reminder that understanding and empathy are as essential as diagnostic clarity.
Production Credits:
Interview conducted, edited, and formatted by the author for this article.
Future Fertility and Medical Outlook
The overwhelming majority of individuals who experience a blighted ovum go on to conceive again and carry healthy pregnancies. Since most cases are random chromosomal events, they rarely indicate systemic reproductive issues. Waiting one menstrual cycle is often recommended for emotional and physical readiness, though extended waiting periods are typically unnecessary.
Recurrent blighted ova are uncommon. If early pregnancy losses repeat, clinicians may suggest genetic counseling or testing. Yet for most, the path forward is straightforward: healing, try again, hope cautiously renewed.
Emotional Recovery
Early pregnancy loss can be invisible to others. There may be no ultrasound photo, no baby bump, no items purchased for a nursery. And yet the loss is profound. People grieve the future they imagined, the heartbeat they expected to hear, and the identity shift toward parenthood that had already begun internally.
Supportive partners, empathetic clinicians, and community resources play vital roles. Grief counseling or support groups may help. Acknowledging the loss openly can validate feelings that otherwise remain unspoken. The absence of an embryo does not diminish the emotional reality of early pregnancy.
Takeaways
- A blighted ovum occurs when a gestational sac forms but an embryo does not.
- Chromosomal abnormalities are the main cause and are typically random.
- Symptoms may mimic a healthy pregnancy due to continued hormone production.
- Diagnosis relies on ultrasound imaging rather than symptoms or hormone levels alone.
- Management options include natural miscarriage, medical treatment, or surgical intervention.
- Most individuals go on to have healthy pregnancies afterward.
- Emotional support and validation are essential parts of recovery.
Conclusion
A blighted ovum represents the quietest form of pregnancy loss—one discovered early, often without warning, in the stillness of a scan room. Its emptiness carries both clinical clarity and emotional weight. But understanding its biological roots helps replace self-blame with perspective: this is a random chromosomal event, not a failure. And while the loss can reshape expectations and temporarily dim hope, it does not define future fertility.
Most people who experience this early miscarriage eventually conceive again and deliver healthy babies. The path between loss and hope is rarely linear, but it is navigable with compassion, clear information, and support. In recognizing both the science and the tenderness of early pregnancy loss, we honor not just the diagnosis but the humanity inside those quiet, unexpected moments.
FAQs
What exactly causes a blighted ovum?
Chromosomal abnormalities in the fertilized egg prevent normal embryonic development, even while the gestational sac continues to grow early on.
Can symptoms alone reveal a blighted ovum?
No. Symptoms often mimic a normal pregnancy. Only ultrasound imaging can confirm the condition.
Does one blighted ovum increase future miscarriage risk?
Generally no. Most people go on to have healthy pregnancies with no long-term fertility issues.
How soon can someone try to conceive again?
Many clinicians suggest waiting one menstrual cycle, mostly for emotional clarity; extended delays are usually unnecessary.
Is a blighted ovum preventable?
No. Because the event is typically due to random chromosomal errors, it cannot be prevented by behavior or lifestyle changes.
References
- Chaudhry, K. (2023). Anembryonic pregnancy (blighted ovum). StatPearls, NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK499938/
- Mayo Clinic Staff. (n.d.). Blighted ovum: Causes and symptoms. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/pregnancy-loss-miscarriage/expert-answers/blighted-ovum/faq-20057783
- Cleveland Clinic. (n.d.). Blighted ovum (anembryonic pregnancy). https://my.clevelandclinic.org/health/diseases/21924-blighted-ovum
- Healthline. (2017). Blighted ovum: Treatment, symptoms, causes, and outlook. https://www.healthline.com/health/pregnancy/blighted-ovum
- Pregnancy, Birth & Baby. (n.d.). Blighted ovum. https://www.pregnancybirthbaby.org.au/blighted-ovum
- International Journal of Reproduction, Contraception, Obstetrics and Gynecology. (2019). Prevalence of blighted ovum in early pregnancy. https://www.ijrcog.org/index.php/ijrcog/article/download/5854/4145