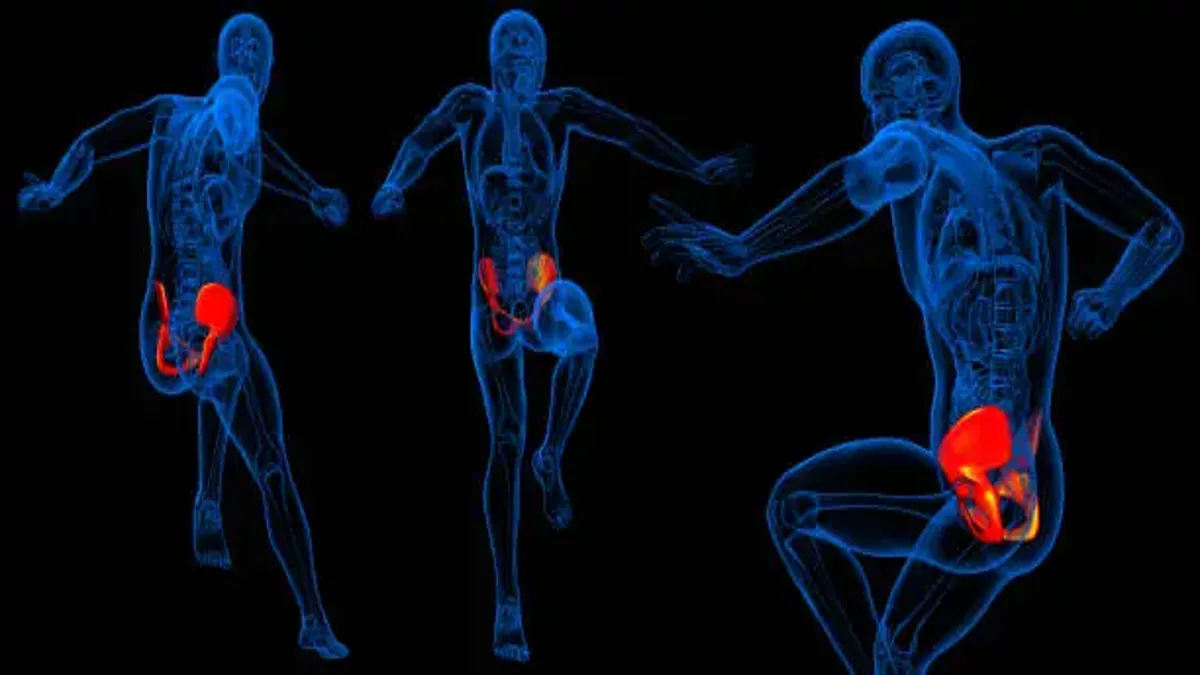
Gluteal tendinopathy has emerged as one of the most common yet frequently misinterpreted causes of persistent outer-hip pain, forcing clinicians and researchers to rethink long-held assumptions about where hip discomfort originates. In the first 100 words: the condition arises not from sudden inflammation but from gradual, degenerative weakening of the gluteus medius and minimus tendons where they anchor to the greater trochanter of the femur. This slow deterioration disrupts hip stability, irritates surrounding structures, and produces a dull, radiating ache that can make side-sleeping, stair climbing, walking, and prolonged sitting enormously difficult. Although many people assume the issue is bursitis or arthritis, research now consistently shows that these tendons — rather than the bursa — are often the primary source of persistent lateral hip pain.
The complexity of gluteal tendinopathy lies in its quiet evolution. Symptoms usually begin subtly — a faint tenderness over the outer hip, stiffness after long walks, or an intermittent discomfort when lying on one side. Over months or years, that minor irritation may progress into sharp pain, disrupted sleep, limping, and difficulty balancing on a single leg. Because the tendons play an essential role in pelvic stabilization, their gradual failure affects not only movement but also posture, gait mechanics, and overall quality of life. Unlike acute injuries, this is a chronic degenerative process that rarely resolves spontaneously and seldom improves through rest alone.
This article examines gluteal tendinopathy through the lens of long-form health reporting: how the condition develops, why it disproportionately affects certain populations, the evolving science behind diagnosis, and the shifting consensus on treatment. It further incorporates clinical insight, expert commentary, and structured comparative data to help readers understand both the biology and lived experience of this underestimated condition.
Understanding Gluteal Tendinopathy
The gluteus medius and gluteus minimus are primary stabilizers of the pelvis, crucial for single-leg stance, walking, stair climbing, and maintaining rotational control of the hip. When their tendons gradually degenerate, microscopic fiber disruption accumulates until the tissue weakens, thickens, or frays. This degenerative process — tendinosis — differs fundamentally from acute inflammation. Rather than swelling or heat, the hallmark is structural decline: weakened collagen, reduced tensile capacity, and impaired load tolerance.
This distinction reshaped the clinical landscape. For decades, most lateral hip pain was labeled “trochanteric bursitis,” assuming that inflammation in the bursa was the principal culprit. Yet medical imaging later revealed that tendon degeneration — not bursal inflammation — appeared far more frequently in chronic cases. As a result, clinicians now increasingly view gluteal tendinopathy as the central driver in what was once lumped under a broader category of greater trochanteric pain.
Because tendons deteriorate slowly, many individuals unknowingly aggravate the problem by repeating small daily stresses: crossing legs while sitting, standing with hip sway, sleeping on one side, or running without adequate strength conditioning. Over time, these patterns load the lateral hip in ways the vulnerable tendon cannot tolerate. The cumulative effect is a cycle of pain that often confuses patients — steady enough to limit daily function but diffuse enough to make self-diagnosis unreliable.
How Gluteal Tendinopathy Differs from Other Causes of Lateral Hip Pain
While gluteal tendinopathy shares anatomical proximity with bursitis or traditional tendinitis, it behaves differently physiologically and clinically. The following table outlines key distinctions:
Comparison of Common Lateral Hip Conditions
| Condition | Pathology | Typical Onset | Response to Rest |
|---|---|---|---|
| Tendinitis | Acute tendon inflammation | Sudden, overuse-related | Often improves with rest/NSAIDs |
| Trochanteric bursitis | Inflamed bursa near greater trochanter | Gradual or sharp onset | Frequently responds to anti-inflammatory care |
| Gluteal tendinopathy | Chronic tendon degeneration | Slow, insidious | Rest alone rarely effective; requires strengthening and load management |
These differences alter treatment choices substantially. A condition driven by degeneration does not respond to strategies meant for inflammation. As one physical medicine specialist notes: “You cannot reduce your way out of a degenerative tendon problem. You must rebuild capacity.”
Another physiotherapist adds: “Patients who rely solely on rest often feel temporary relief, only to relapse because the tendon remains weak and intolerant to everyday loads.”
And a sports rehabilitation researcher emphasizes: “Strengthening is not just therapeutic — it is essential. Tendons demand progressive load to reorganize and recover.”
Symptoms and Daily Life Disruption
The hallmark symptom of gluteal tendinopathy is a deep, aching pain along the outer aspect of the hip, centered over the greater trochanter. Many describe it as a pressure pain, especially when lying on the affected side, which leads to disturbed or fragmented sleep. Activities requiring single-leg loading — stepping up, rising from a chair, prolonged standing, or walking long distances — intensify the ache.
The discomfort may radiate down the outer thigh, sometimes mimicking sciatica. Unlike joint arthritis, however, the pain tends not to center in the groin and does not consistently accompany stiffness inside the hip joint. Sufferers often adopt compensatory movements: shifting weight away from the painful side, avoiding stairs, or leaning their torso to reduce load. These adaptations, while instinctive, can perpetuate the problem by weakening the hip abductors further.
Over time, the condition can impose meaningful constraints on daily life: limiting exercise, reducing participation in activities, and increasing fear of movement. The emotional toll is equally real. Chronic hip pain frequently leads to frustration, sleep deprivation, and reduced confidence in mobility — especially when previous diagnoses failed to account for the underlying tendon degeneration.
Diagnostic Process
A typical clinical examination begins with palpation over the greater trochanter. Localized tenderness, especially when paired with pain during resisted abduction or specific rotation tests, strongly suggests tendon involvement. Clinicians may perform tests that place compressive or tensile stress on the tendons to reproduce symptoms.
Imaging — particularly ultrasound or MRI — can support diagnosis by revealing tendon thickening, partial tearing, or characteristic degenerative changes. These modalities also help distinguish gluteal tendinopathy from referred pain originating in the lumbar spine or from intra-articular hip conditions.
Despite increasing awareness, misdiagnosis remains common. Many individuals are initially told they have bursitis, muscle strain, or nonspecific hip pain. Recognizing the pattern of tendon degeneration helps ensure earlier, more accurate intervention — and avoids ineffective treatments that mask symptoms but fail to restore load capacity.
Treatment Principles
The cornerstone of modern treatment is progressive strengthening combined with load management. Unlike inflammatory conditions that respond to rest, degenerative tendons require deliberate mechanical stimulus to rebuild. Effective treatment generally combines:
- Progressive resistance training
- Education on posture, sleeping positions, and activity modification
- Gradual re-exposure to load-bearing activities
- Avoidance of compressive positions such as crossing legs or leaning the hip
Although some individuals seek injections, passive treatments alone rarely deliver long-term improvement. Corticosteroids may briefly reduce pain, but because the tendon remains degraded, symptoms frequently return once activity resumes. In contrast, strengthening programs restore tendon stiffness, improve hip stability, and help patients tolerate functional activities again.
Surgical options are reserved for rare, severe cases — typically involving large partial tendon tears or structural failure unresponsive to months of rehabilitation. Even then, postoperative success depends heavily on continued strengthening.
Table: Common Treatment Options and Their Roles
| Treatment | Purpose | Strengths | Limitations |
|---|---|---|---|
| Strengthening program | Rebuild tendon capacity | Best long-term outcomes | Requires time, consistency |
| Load management | Reduce mechanical irritation | Immediate symptom relief | Must pair with strengthening |
| Corticosteroid injection | Temporary pain reduction | Short-term relief | No long-term tendon benefit |
| Shockwave therapy | Adjunct stimulus | Helps select chronic cases | Not a standalone solution |
| Surgery | Repair severe tendon damage | Reserved for advanced degeneration | Invasive, lengthy recovery |
The consensus remains firm: strengthening is the only intervention consistently linked to sustained functional improvement.
Interview Section
“The Hip That Wouldn’t Quiet Down”
Date: Early morning, autumn
Location: A quiet rehabilitation clinic
Atmosphere: Low light, soft hum of equipment, faint smell of disinfectant
The interviewer introduces herself to Dr. L., a rehabilitation specialist known for her work with chronic tendon conditions. She sits across a small wooden table, notebook open, as the doctor folds her hands — calm, deliberate, analytical.
Scene-Setting Paragraph:
In the dim hallway behind the treatment room, patients shuffle in and out of appointment slots. Some walk gingerly, others confidently. Dr. L. greets each with the same measured warmth. She has spent nearly a decade reframing how lateral hip pain is understood, insisting that what many dismiss as “simple bursitis” is often a deeper structural story. Today, she reflects on the complexities and misconceptions surrounding gluteal tendinopathy.
Q&A
Q: When patients come in describing lateral hip pain, what’s the first misconception you encounter?
A: She pauses, tapping her pen gently. “Most assume inflammation — something swollen that needs calming. But in chronic cases, we’re usually dealing with degeneration. That requires rebuilding, not resting.”
Q: Why does the condition persist for months or years?
Dr. L. leans back. “Because people keep loading the tendon in the very ways that irritate it — sleeping on that side, crossing their legs, standing with hip drop. Without correcting mechanics, the cycle continues.”
Q: What is the emotional toll of chronic hip pain?
She sighs softly. “It disrupts sleep. It limits mobility. People lose trust in their bodies. Many feel dismissed because prior treatments focused on the bursa or inflammation rather than the real problem.”
Q: What makes rehabilitation effective when done properly?
“The tendon responds to progressive mechanical load. It reorganizes. Patients often fear strengthening at first, but when they commit, their confidence returns.”
Q: What is the most important thing you tell newly diagnosed patients?
She smiles. “Patience. Tendons heal slowly — not dramatically, but steadily. The goal is resilience, not quick fixes.”
Post-Interview Reflection
Walking out of the clinic, the steady rhythm of the doctor’s words lingers. Her insistence on slow rebuilding rather than rapid relief reflects a broader truth about chronic musculoskeletal pain: the body changes gradually, and recovery often requires the same kind of time, structure and persistence.
Production Credits:
Interview conducted, transcribed and edited by the author.
Takeaways
- Gluteal tendinopathy stems from tendon degeneration, not acute inflammation.
- Pain typically centers on the outer hip and worsens with weight-bearing.
- Imaging can confirm tendon changes and rule out alternate sources.
- Strengthening and load management are the only consistently effective long-term treatments.
- Sleep modification, posture changes and progressive resistance training support recovery.
- Short-term interventions without strengthening rarely prevent recurrence.
Conclusion
Gluteal tendinopathy is a deceptively quiet condition — one that begins with subtle irritation and gradually infiltrates sleep, movement and daily function. Its slow onset and overlapping symptoms long obscured its true nature, resulting in years of misdiagnosis and misguided treatment. Yet as research reframes lateral hip pain through the lens of tendon degeneration, clinicians increasingly emphasize rebuilding rather than resting. Strengthening, education, and thoughtful load management now form the backbone of effective care.
The condition remains challenging, not because it is unmanageable but because it demands time, patience and structured rehabilitation. For many patients, recovery is both physical and psychological — a return to trust in their movement, in their body’s ability to withstand load, and in the possibility of pain-free mobility. With clearer understanding and consistent treatment, gluteal tendinopathy need not dictate years of discomfort. Instead, it can become a pathway toward stronger, more resilient movement.
FAQs
1. Can gluteal tendinopathy cause radiating pain?
Yes. Pain can spread down the outer thigh, often mimicking nerve-related discomfort, but usually remains lateral rather than deep in the groin.
2. Is rest enough to treat this condition?
No. Because the tendon is degenerative, rest may ease symptoms temporarily but does not rebuild tendon structure.
3. How long does strengthening take to show improvement?
Many patients notice functional gains in 8–12 weeks, though full rehabilitation may take several months.
4. Should I stop walking or exercising?
Not entirely. Activity should be modified, not abandoned. Guided progressive loading is essential to healing.
5. Does lying on the affected side worsen symptoms?
Yes. Side-lying increases compressive forces on the tendon and often intensifies night pain.
References
- Cleveland Clinic. (n.d.). Gluteal tendinopathy. https://my.clevelandclinic.org/health/diseases/22960-gluteal-tendinopathy
- PhysioPedia. (n.d.). Gluteal tendinopathy overview. https://www.physio-pedia.com/Gluteal_Tendinopathy
- Nature. (2024). Exercise-based therapy outcomes for gluteal tendinopathy. https://www.nature.com/articles/s41598-024-53283-x
- JOSPT. (2015). Greater trochanteric pain syndrome redefined. https://www.jospt.org/doi/10.2519/jospt.2015.5829
- East Sussex Healthcare NHS. (2019). Patient information: Gluteal tendinopathy. https://www.esht.nhs.uk/wp-content/uploads/2019/07/0746.pdf
- Sciencedirect. (2025). Rehabilitation principles for hip tendinopathy. https://www.sciencedirect.com/science/article/pii/S1836955325000177